This video lecture offers a comprehensive exploration of bone health within the broader framework of holistic wellness. It connects the anatomy and physiology of bones to lifestyle factors, emphasizing the intricate links between physical, mental, and spiritual health. Starting with a review of prior wellness topics such as balance, breathing, and acupressure meridians, I strived to situate bone health in a systems view, explaining how weak bones affect balance and mobility. Key causes of bone weakening, such as sedentary lifestyle, poor diet, hormonal changes, genetics, stress, and insufficient vitamin D, are examined in detail.
The lecture highlights the importance of regular exercise, including weight-bearing activities, Tai Chi, yoga, and functional fitness, to stimulate bone remodeling and maintain strength across the lifespan. Additionally, it addresses the role of calcium, vitamin D, and supplements, as well as medical interventions like acupuncture and TENS (Transcutaneous Electrical Nerve Stimulation) for pain management. I spoke of integrating traditional Chinese medicine concepts, stress benefits, and mindful breathing into the discussion, reinforcing a holistic view of health. Practical tips for maintaining bone integrity, improving balance, and avoiding falls are offered along with a call for consistent, varied physical activity as the cornerstone of healthy aging. The video finishes with a Q&A style wrap-up that stresses individual variability and the importance of personalized healthcare guidance.
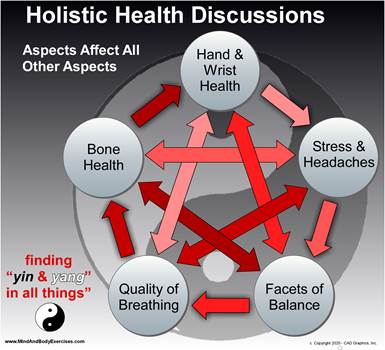
Interconnectedness of Systems: The presentation emphasizes that bone health is not isolated but deeply intertwined with muscular, neurological, and even spiritual health. For example, weak bones increase fall risk, which can cascade into fractures and loss of mobility, illustrating the systemic nature of health challenges. The concept of yin and yang underscores the balance between internal wellness and external fitness, highlighting that physical strength alone is insufficient without emotional and mental well-being. This integrated approach reflects contemporary holistic health paradigms.
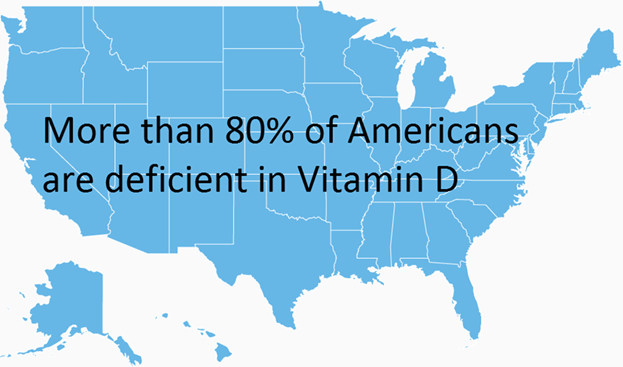
Vitamin D’s Crucial Role and Sunlight Exposure: A significant insight is the critical role of vitamin D in calcium absorption and bone integrity. I highlighted how modern lifestyles have evolved our indoor activities, sunscreen use, geographic latitude, and seasonal changes, contributing to widespread vitamin D deficiency. This deficiency links to multiple conditions including osteoporosis, osteomalacia, rickets, and compromised immunity. The discussion about timing and duration of sun exposure elucidates practical strategies to optimize vitamin D without risking skin damage, encouraging mindful balance.
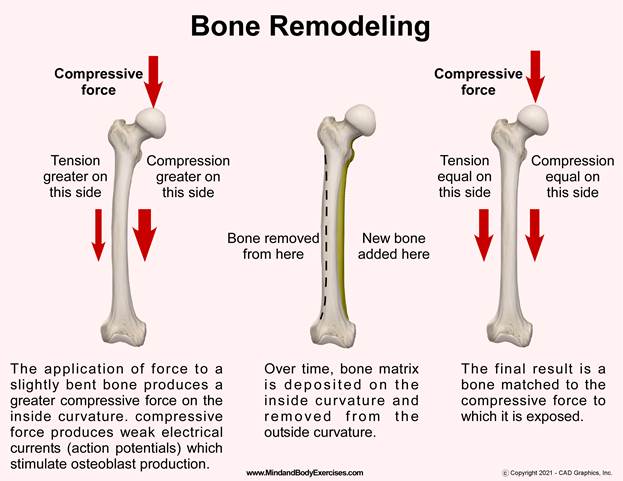
Exercise as a Primary Modulator of Bone Strength: Wolf’s Law explains how mechanical strain on bones via muscle tension prompts remodeling and strengthening. The presentation breaks down exercise types, from gentle Tai Chi to rigorous weight training and their suitability across age groups, stressing the importance of consistency and variety. I caution that overly repetitive or limited-exercise regimens may enhance one skill set but neglect others (e.g., flexibility, cardiovascular health), advocating for a multi-dimensional fitness approach. Use of weighted vests, wrist weights, and grip exercises further illustrates how progressive tension can be tailored to individual capacity.
Balance and Grip Strength are Vital for Injury Prevention: Falls are a leading cause of fractures in older adults; thus, balance training and grip strength are crucial preventive measures. The lecture connects muscle strength, proprioception, and neuromuscular coordination as key to maintaining postural stability. Grip strength matters not only for daily function but also as an indicator of overall health and balance recovery capability during falls, making it a practical focus area for exercise programs.
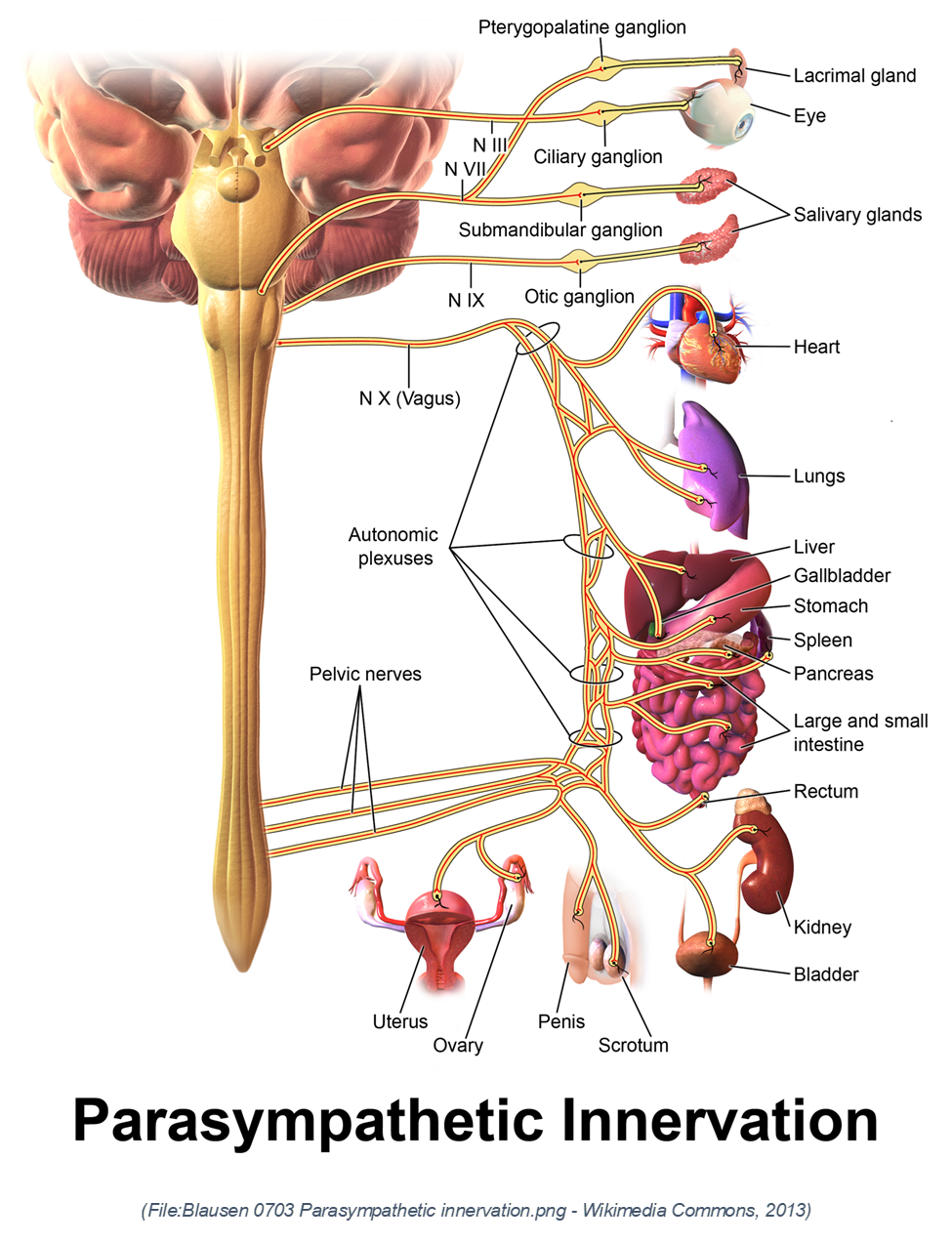
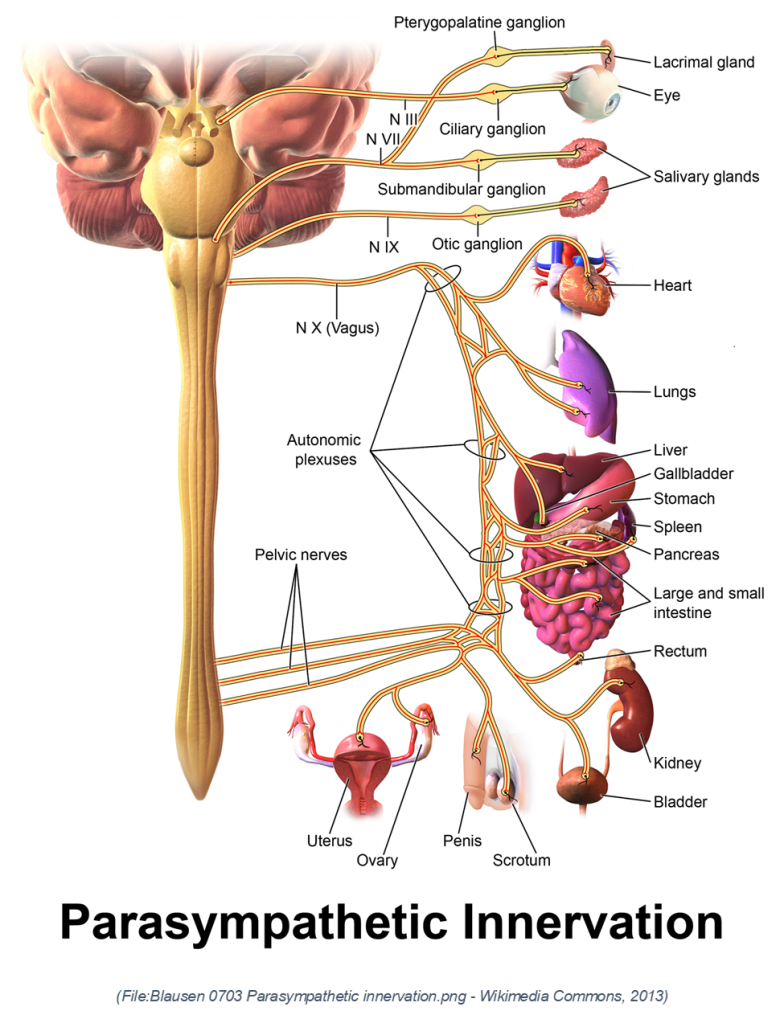
Holistic Fitness and Organ Health through Movement: Unlike traditional fitness focused solely on muscles and cardiovascular systems, the talk introduces the idea that practices like Tai Chi and yoga actively stimulate internal organs by promoting diaphragmatic movement and circulation. This ‘soft fitness’ concept aligns with traditional Chinese medicine, promoting blood flow and nervous system activation via acupressure meridians. This insight expands the definition of fitness towards holistic bodily integration and organ vitality.
Complementary Modalities for Pain and Bone Health: The acceptance and use of acupuncture, acupressure, and TENS units are discussed as effective tools for pain relief without drugs, especially for arthritis and bone-related discomfort. While these do not cure structural issues, their value in managing symptoms and enabling movement enhances quality of life. The lecture also discusses complexities around calcium supplements and pharmaceuticals, emphasizing nutritional balance and caution due to potential side effects like kidney stones or brittle bones.
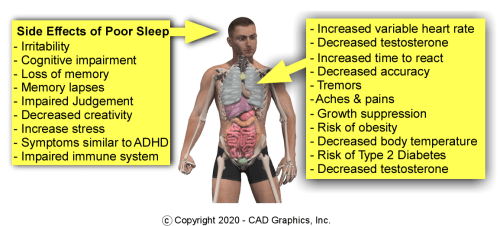
Stress Hormones Impact Bone Remodeling: Chronic stress elevates cortisol levels, which negatively affects bone formation and increases breakdown, illustrating the biochemical pathways connecting emotional health and bone physiology. The analogy to a microwave running empty underscores how unrelenting stress can burn out the system. Incorporating stress management, mindful breathing, and spiritual awareness into daily practice is thus integral to sustaining bone health, emphasizing mind-body unity in disease prevention and health promotion.
Highlights
- Holistic health views bones as interconnected with muscles, organs, and energy meridians.
- Vitamin D deficiency is widespread and profoundly impacts bone strength and immunity.
- Weight-bearing exercise and diverse physical activity stimulate bone remodeling at any age.
- Balance, grip strength, and neuromuscular coordination are critical for fall and injury prevention.
- Soft movement practices like Tai Chi and yoga engage muscles and organs for whole-body wellness.
- Acupuncture and TENS offer non-pharmaceutical options for managing bone-related pain.
- Stress and mental health considerably affect bone physiology via hormonal pathways like cortisol.
I feel that this discussion offers an in-depth, well-rounded discussion on bone health, rooting it firmly in a holistic wellness model. It broadens the narrative beyond simple calcium intake or exercise regimens, weaving in mental health, stress, spirituality, and modern lifestyle factors. Practical, evidence-backed advice coupled with traditional medicine knowledge and personal anecdotes make it accessible. Viewers are encouraged to adopt a varied, consistent exercise routine, mind their nutrition and sunlight exposure, manage stress, and consider complementary therapies to maintain strong bones and overall vitality through aging.