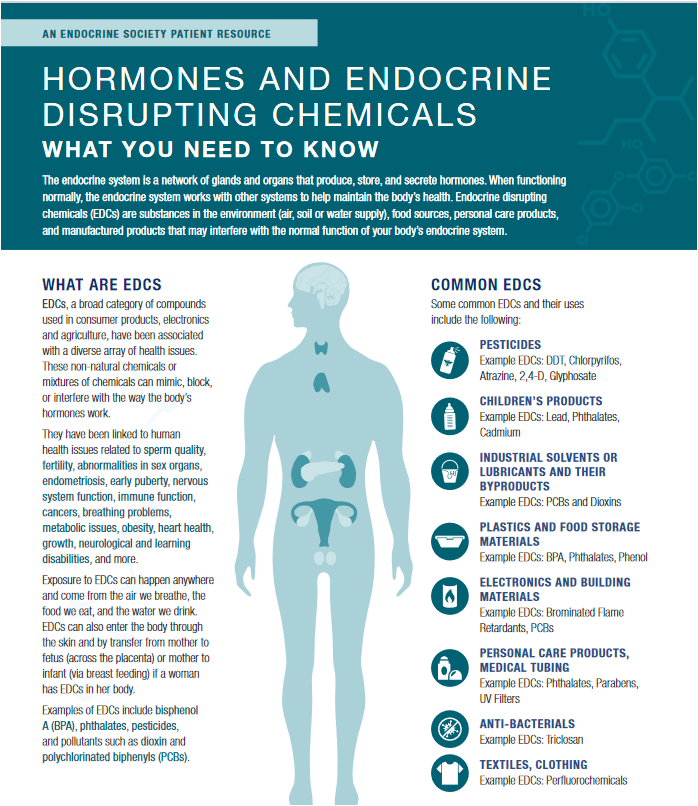
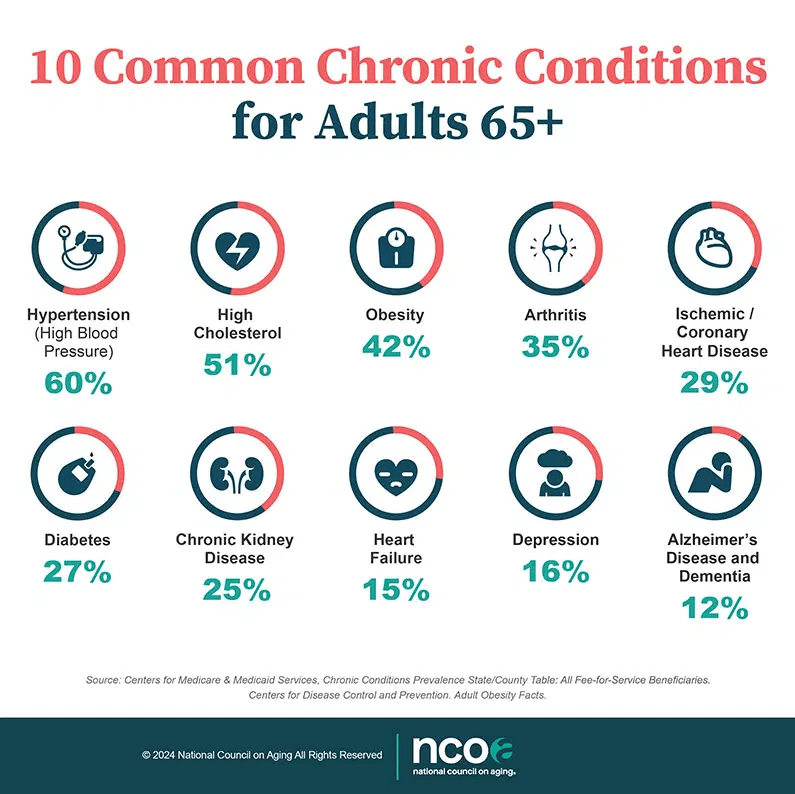
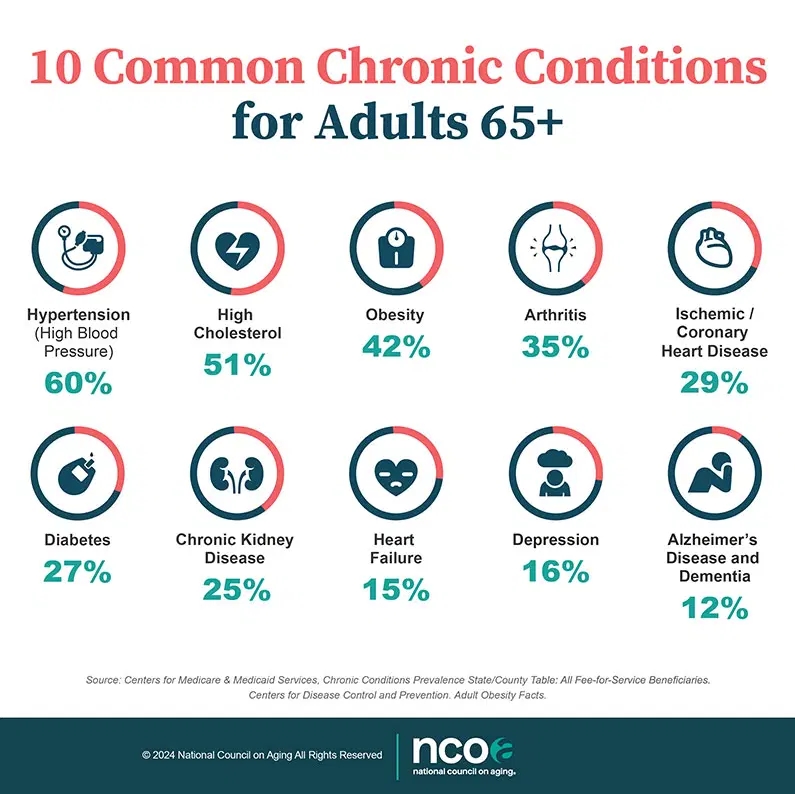
Recently I presented a 3-session discussion of managing chronic pain and various health conditions without relying heavily on pharmaceuticals. Drawing on over four decades of experience in fitness, wellness, and martial arts, I shared practical alternatives for alleviating chronic pain, enhancing overall health, and addressing root causes of illness through natural and holistic methods. The presentation emphasizes lifestyle changes such as regular exercise, proper nutrition, adequate sleep, positive mindset, and maintaining good posture. In addition to physical activity, I introduced various therapies from traditional Chinese medicine like acupuncture, cupping, and herbal treatments, alongside modern tools such as massage guns, acupressure blankets, TENS units, and topical applications like Biofreeze and herbal extracts and oils.
This talk also highlights the important role of breathing techniques and managing thoughts and emotions to influence bodily health, noting the body-mind connection reflected in how emotions such as fear and anger affect organ function. I stressed the importance of building health-supportive habits, acknowledged the challenge of post-traumatic growth, and discussed the nuanced use of heat and cold therapies. Practical advice on selecting and safely using equipment and topical treatments is interwoven with cautions about chemical ingredients and the need for professional guidance when appropriate.
Traditional Chinese medicine explanations include the theory of meridians and fascia as pathways for energy and healing, while acknowledgment of the placebo effect underscores individual variability in treatment success. The presentation culminates with a discussion on herbal remedies and CBD products, encouraging personal experimentation with proper research and awareness of one’s unique constitution. Finally, I outlined future classes focusing on exercises for specific pain areas, breathing techniques, and addressing common ailments such as headaches.
Highlights
- 🌿 Emphasis on managing chronic pain naturally through lifestyle changes and holistic methods.
- 🧘♂️ Importance of regular exercise, stretching, and posture correction to alleviate joint and muscle pain.
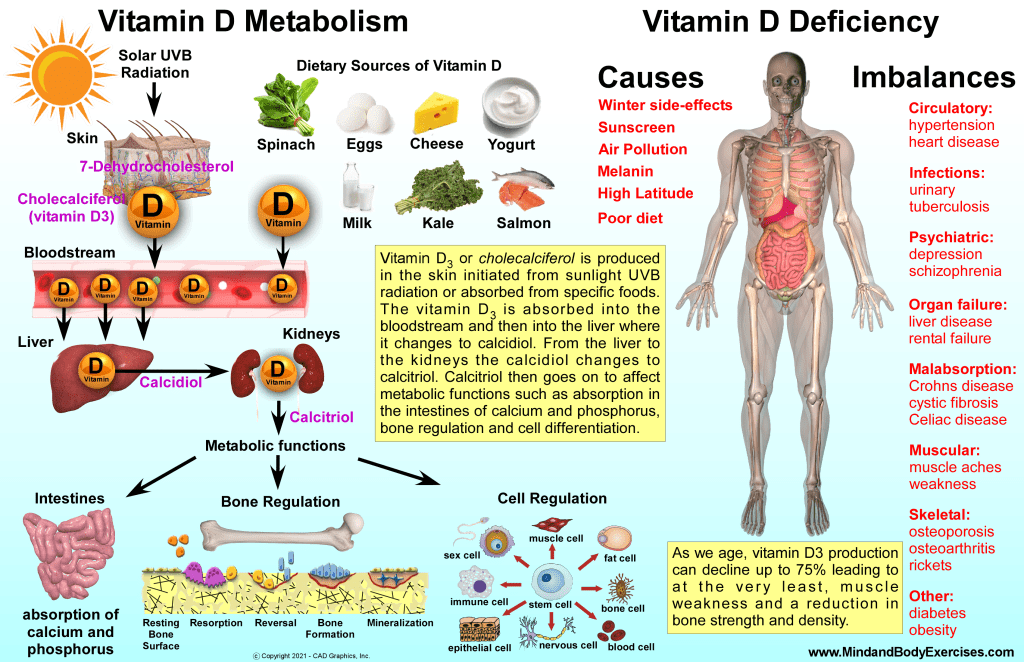
- 🌞 Balanced exposure to sunlight recommended for overall health despite skin cancer concerns.
- 🌬️ Deep, nasal breathing techniques help regulate hormones and reduce stress.
- 💆♀️ Overview of traditional Chinese medicine therapies such as acupuncture, cupping, and reflexology.
- ⚡ Introduction of modern tools like massage guns and TENS units for targeted pain relief.
- 🌱 Discussion of herbal remedies and CBD products with a focus on personal research and safety.
Key Insights
- 🌟 Holistic Approach to Chronic Pain Management: The presentation advocates a multi-faceted strategy that goes beyond drugs, focusing on physical activity, nutrition, sleep, mental health, and social connection. Chronic pain is not treated solely as a symptom requiring pills but as a condition that benefits from addressing root causes like posture, mobility, and emotional well-being.
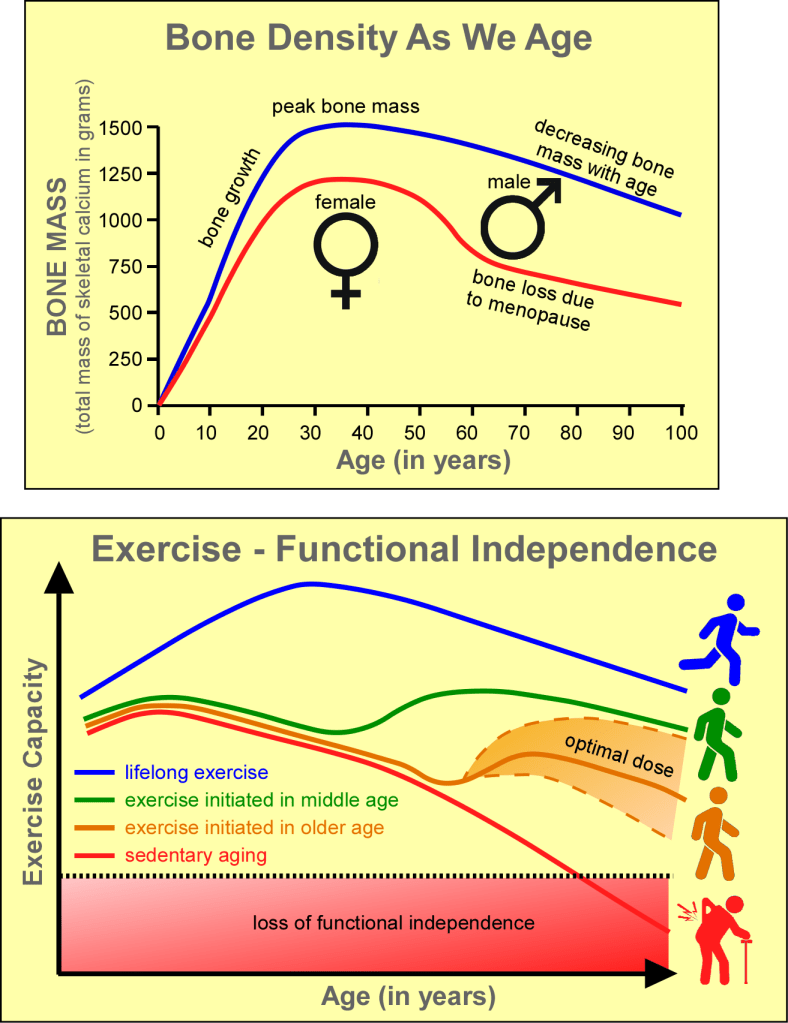
- 💪 Exercise as a Foundation of Health: Regular, thoughtful exercise not only builds strength and flexibility but also aids in maintaining joint integrity and reducing inflammation. Tailored rehabilitation exercises for injury-prone areas such as knees and back show how specific movements can promote healing and prevent surgery, underscoring the preventive value of physical training.
- 🌞 Sunlight’s Dual Role: Despite warnings about sun exposure, moderate sunlight early in the day is beneficial for vitamin D synthesis and overall well-being. This nuanced advice counters extreme avoidance and highlights how balanced choices support immune function and energy metabolism.
- 🧠 Mind-Body Connection Through Thought and Emotion: The concept that emotions influence physical health is grounded in both traditional Asian medicine and modern science. Chronic fear, anger, and depression affect hormone and nervous system balance, which in turn impacts organ health and pain perception. Cultivating positive attitudes is presented as an essential part of holistic health care.
- 🧘 Breathing as a Regulatory Tool: Emphasizing nasal breathing, I explained its biological effects on the nervous system’s fight-or-flight response and hormone regulation. It’s a simple, often overlooked method to enhance relaxation, improve circulation, and support natural healing processes by shifting the body into a rest-and-digest state.
- 🌿 Traditional Chinese Medicine and Modern Integration: The explanation of meridian theory in relation to fascia and connective tissue bridges ancient concepts with current anatomical understanding. Techniques like acupuncture, cupping, and acupressure stimulate circulation and nervous system responses, and while their scientific basis is still debated, many find them effective. The placebo effect is recognized as a legitimate contributor to therapeutic outcomes.
- ⚙️ Safe and Informed Use of Therapeutic Tools and Topicals: Modern devices like massage guns and TENS units can provide effective relief when used properly, but self-education and professional guidance are critical to avoid injury. Similarly, topical treatments like Biofreeze and traditional herbal liniments are recommended with caveats regarding chemical content and appropriate application to prevent adverse reactions.
- 🌱 Individual Variability and Habit Formation: Chronic pain management is highly personalized. What works for one person might not work for another, which places importance on trying different methods and establishing consistent habits to evaluate effectiveness. The 21-day habit-building model is cited to encourage persistence and gradual lifestyle change.
- 🌿 Herbal Medicine and CBD’s Mixed Efficacy: Herbal remedies such as ashwagandha and valerian root, alongside emerging treatments like CBD oil, show promise but require careful individual assessment and research. The overlap with placebo effects means patients must remain open-minded yet discerning, guided by their body’s responses and external advice.
- 🩺 Discerning Between Muscle and Nerve Pain: Understanding the distinction between muscular discomfort and nerve-related pain is key to selecting appropriate therapies. For example, nerve pain may radiate and be treated with different techniques compared to localized muscle soreness, necessitating professional diagnosis to optimize treatment choices.
- 🔥 Heat vs. Cold Therapy Nuances: The presentation challenges simplistic views on hot and cold treatment by discussing recent medical perspectives on risks and timing. Cold is beneficial immediately post-injury to reduce inflammation but can cause cell damage if prolonged, while heat aids recovery after inflammation subsides, supporting personalized and time-sensitive application.
- 🌱 Post-Traumatic Growth Emphasized Over Syndrome: Rather than dwelling on trauma as a limiting factor, I frame it as an opportunity for growth. Adopting this mindset fosters resilience, encouraging individuals to engage in rehabilitation, self-care, and lifestyle changes despite past injuries or stressors contributing to chronic pain.
- 🤝 Value of Social Connection and Mental Health Support: Being part of a supportive community, such as a health class or social network, can distract from pain and enhance feelings of well-being. This social support acts synergistically with physical treatment and mental health practices to bolster overall recovery and health maintenance.
In conclusion, my video offers a rich and practical resource for anyone seeking alternatives or complements to pharmaceutical pain management. It integrates ancient wisdom with contemporary tools and scientific insights, advocating for an active, informed, and individualized approach to chronic pain and health challenges. The emphasis on self-care, preventive habits, and understanding the body-mind interplay positions viewers to take more control of their well-being without over-dependence on medication.