Throughout history, some products initially approved by regulatory agencies such as the U.S. Food and Drug Administration (FDA) and the Environmental Protection Agency (EPA) have later been found to pose risks to human health and the environment. While human error is sometimes unavoidable, minimizing it is crucial for public safety and welfare. From pharmaceuticals to household products, these instances underscore the importance of thorough testing and evaluation. This article examines notable cases such as thalidomide, DDT, and OxyContin, and discusses strategies to prevent similar issues in the future.
Thalidomide: The Drug That Never Reached the U.S. (Officially)
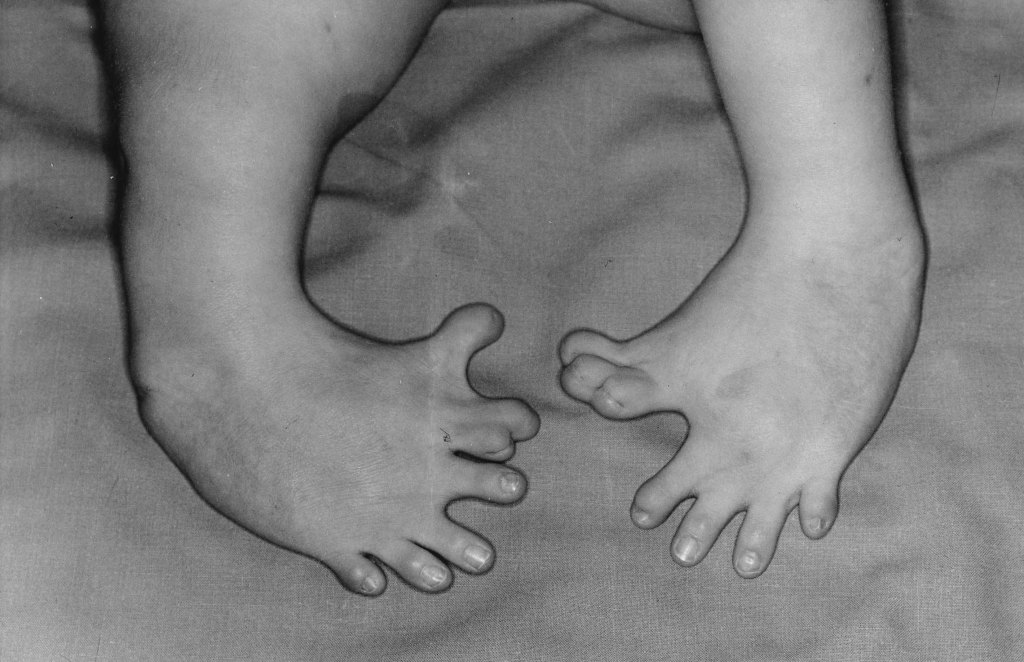
Thalidomide was introduced in the 1950s by the German company Chemie Grünenthal as a sedative and treatment for morning sickness in pregnant women. It was marketed in Europe, Canada, and other countries as a completely safe medication. However, by the late 1950s, a significant number of children were born with severe congenital disabilities, including missing or deformed limbs, organ damage, and other critical conditions (Kim & Scialli, 2011).
Why Wasn’t Thalidomide Approved in the U.S.?
The pharmaceutical company submitted the drug for FDA approval, but Dr. Frances Kelsey, a physician and pharmacologist at the FDA, halted its approval. She requested additional safety data due to suspected potential hazards. As a result of her diligence, the United States avoided a significant public health disaster (Daemmrich, 2004).
Although not approved, certain U.S. doctors were able to access the drug through experimental trials. Approximately 17 children in the United States were born with birth defects associated with thalidomide (Kim & Scialli, 2011). While this figure is relatively small compared to the over 10,000 cases worldwide, it underscores the risks involved with unregulated drug distribution. Thalidomide resulted in significant modifications to drug approval processes globally, including enhanced testing for fetal safety and stricter FDA guidelines that continue today (Daemmrich, 2004).
DDT: The Miracle Pesticide Turned Environmental Nightmare
DDT (Dichlorodiphenyltrichloroethane) was introduced in the 1940s as a pesticide to address malaria and typhus. It was widely used by the U.S. military during World War II and subsequently gained popularity in agriculture and public health programs (Eskenazi et al., 2009).
By the 1960s, concerns about the environmental and health impacts of DDT became more prominent. Rachel Carson’s seminal book, Silent Spring (1962), documented the bioaccumulation of DDT in wildlife, which resulted in the thinning of bird eggshells and contributed to the near-extinction of bald eagles. Additionally, Carson highlighted the potential carcinogenic effects of DDT on humans (Carson, 1962).
DDT was prohibited in the United States in 1972; however, it continues to be utilized in certain regions globally for malaria control (Eskenazi et al., 2009).
OxyContin & the Opioid Epidemic: A Tragic Case of Corporate Deception
In 1996, Purdue Pharma launched OxyContin, promoting it as a non-addictive pain medication. The Food and Drug Administration (FDA) approved the drug based on Purdue’s assertions that its time-release formulation would mitigate the potential for abuse (Van Zee, 2009).
OxyContin has been associated with high addiction rates, and its widespread prescription contributed to a national opioid crisis. Purdue Pharma and other manufacturers later faced lawsuits, with evidence suggesting that they did not fully disclose the drug’s risks to doctors and regulators (Van Zee, 2009).
The opioid crisis has led to over 500,000 overdose deaths in the United States since the late 1990s (Uncovering the Opioid Epidemic, n.d.). Although current opioid regulations are significantly stricter, the consequences of the crisis persist.
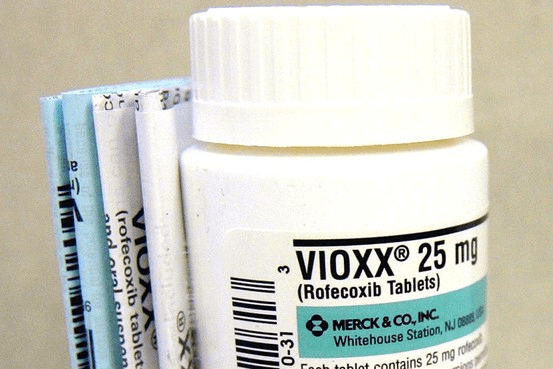
Vioxx: The Painkiller That Led to Heart Attacks
Vioxx (Rofecoxib), a medication for arthritis, was released in 1999 and marketed as an alternative to older anti-inflammatory drugs. Subsequent studies indicated that Vioxx was associated with an increased risk of heart attacks and strokes (Graham et al., 2005).
By the time Vioxx was withdrawn from the market, it is estimated that 20 million Americans had taken the drug. Research later published in the medical journal Lancet estimates that 88,000 Americans experienced heart attacks due to taking Vioxx, with 38,000 fatalities (Prakash, 2007). This case underscored the inadequacy of drug companies in disclosing safety risks and led to the implementation of more stringent post-market drug surveillance policies.
Other Notable Cases of “Safe” Products That Became Harmful
🔹 Tobacco: Once promoted as doctor-approved, later linked to lung cancer and heart disease (Centers for Disease Control and Prevention (US), 2014)
🔹 Lead Paint & Leaded Gasoline: Used for decades despite known toxicity, leading to widespread neurological damage in children (Needleman, 2004).
🔹 Asbestos: Used in construction for insulation but later found to cause mesothelioma and lung disease (Bolan et al., 2023)
🔹 Baby Powder (Talc): Contaminated with asbestos, leading to lawsuits over ovarian cancer risks (Cramer et al., 2015)
🔹 Frontal Lobotomies: Once considered a treatment for mental illness, but resulted in severe cognitive impairment and even death (Faria, 2013)
🔹 Agent Orange: A herbicide used during the Vietnam War, later linked to cancer and birth defects (Stellman & Stellman, 2018)
🔹 PFAS (“Forever Chemicals”): Found in water supplies and linked to cancer, infertility, and immune disorders (Ayodele & Obeng-Gyasi, 2024)
Lessons Learned & How to Protect Ourselves Today
Question Corporate Claims: Research beyond marketing as companies may prioritize profits over safety.
Demand Rigorous Testing: Ensure drugs and chemicals undergo long-term studies before use.
Advocate for Transparency: Pressure is crucial to release hidden data on harmful products.
Support Independent Research: Prioritize independent, peer-reviewed research over industry-funded studies.
Stay Informed: Be vigilant about new risks like microplastics in food and AI-driven medical decisions.
References
Ayodele, A., & Obeng-Gyasi, E. (2024). Exploring the Potential Link between PFAS Exposure and Endometrial Cancer: A Review of Environmental and Sociodemographic Factors. Cancers, 16(5), 983. https://doi.org/10.3390/cancers16050983
Bolan, S., Kempton, L., McCarthy, T., Wijesekara, H., Piyathilake, U., Jasemizad, T., Padhye, L. P., Zhang, T., Rinklebe, J., Wang, H., Kirkham, M., Siddique, K. H., & Bolan, N. (2023). Sustainable management of hazardous asbestos-containing materials: Containment, stabilization and inertization. The Science of the Total Environment, 881, 163456. https://doi.org/10.1016/j.scitotenv.2023.163456
Carson, R. (1962). Silent spring. Houghton Mifflin.
Centers for Disease Control and Prevention (US). (2014). The Health Consequences of Smoking—50 years of progress. NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK179276/
Cramer, D. W., Vitonis, A. F., Terry, K. L., Welch, W. R., & Titus, L. J. (2015). The association between Talc use and ovarian cancer. Epidemiology, 27(3), 334–346. https://doi.org/10.1097/ede.0000000000000434
Daemmrich, A. (2004). Pharmacopolitics: Drug regulation in the United States and Germany. UNC Press Books.
Eskenazi, B., Chevrier, J., Rosas, L. G., Anderson, H. A., Bornman, R., Bouwman, H., … & Warner, M. (2009). The Pine River statement: Human health consequences of DDT use. Environmental Health Perspectives, 117(9), 1359-1367.
Faria, M. (2013). Violence, mental illness, and the brain – A brief history of psychosurgery: Part 1 – From trephination to lobotomy. Surgical Neurology International, 4(1), 49. https://doi.org/10.4103/2152-7806.110146
File:NCP14053.jpg – Wikimedia Commons. (n.d.). https://commons.wikimedia.org/wiki/File:NCP14053.jpg
Graham, D. J., Campen, D., Hui, R., Spence, M., Cheetham, C., Levy, G., Shoor, S., & Ray, W. A. (2005). Risk of acute myocardial infarction and sudden cardiac death in patients treated with cyclo-oxygenase 2 selective and non-selective non-steroidal anti-inflammatory drugs: nested case-control study. The Lancet, 365(9458), 475–481. https://doi.org/10.1016/s0140-6736(05)17864-7
Kim, J. H., & Scialli, A. R. (2011). Thalidomide: The tragedy of birth defects and the effective treatment of disease. Toxicological Sciences, 122(1), 1-6.
Needleman, H. (2004). Lead poisoning. Annual Review of Medicine, 55(1), 209–222. https://doi.org/10.1146/annurev.med.55.091902.103653
Prakash, S. (2007, November 10). Timeline: The rise and fall of Vioxx. NPR. https://www.npr.org/2007/11/10/5470430/timeline-the-rise-and-fall-of-vioxx
Rockoff, J. (2009, November 24). Vioxx and heart attack linked in 2001. WSJ. https://www.wsj.com/articles/SB10001424052748704779704574554071807123380
Stellman, J. M., & Stellman, S. D. (2018). Agent Orange during the Vietnam War: the lingering issue of its civilian and military health impact. American Journal of Public Health, 108(6), 726–728. https://doi.org/10.2105/ajph.2018.304426
Van Zee, A. (2009). The promotion and marketing of OxyContin: Commercial triumph, public health tragedy. American Journal of Public Health, 99(2), 221-227. https://doi.org/10.2105/AJPH.2007.131714
Uncovering the opioid epidemic. (n.d.). https://www.cdc.gov/museum/pdf/cdcm-pha-stem-uncovering-the-opioid-epidemic-lesson.pdf
I look forward to further sharing more of my message by partnering with hospitals, wellness centers, VA centers, schools on all levels, businesses, and individuals who see the value in building a stronger nation through building a healthier population.
I also have hundreds of FREE education video classes, lectures, and seminars available on my YouTube channel at:
https://www.youtube.com/c/MindandBodyExercises
Many of my publications can be found on Amazon at:
http://www.Amazon.com/author/jimmoltzan
My holistic health blog is available at:
https://mindandbodyexercises.wordpress.com/
http://www.MindAndBodyExercises.com
Mind and Body Exercises on Google: https://posts.gle/aD47Qo
Jim Moltzan
407-234-0119